GLP-1 medications have quickly become one of the most talked-about topics in healthcare, with more than 500,000 providers prescribing these medications in 2025, reflecting rapid expansion across clinical settings, according to the IQVIA analysis reported by Becker’s Hospital Review.
Employees are asking about them in increasing numbers. Physicians are prescribing them more often. Employers are being pulled into the conversation, whether they are ready or not.
To understand why, it helps to start with what these medications actually do.
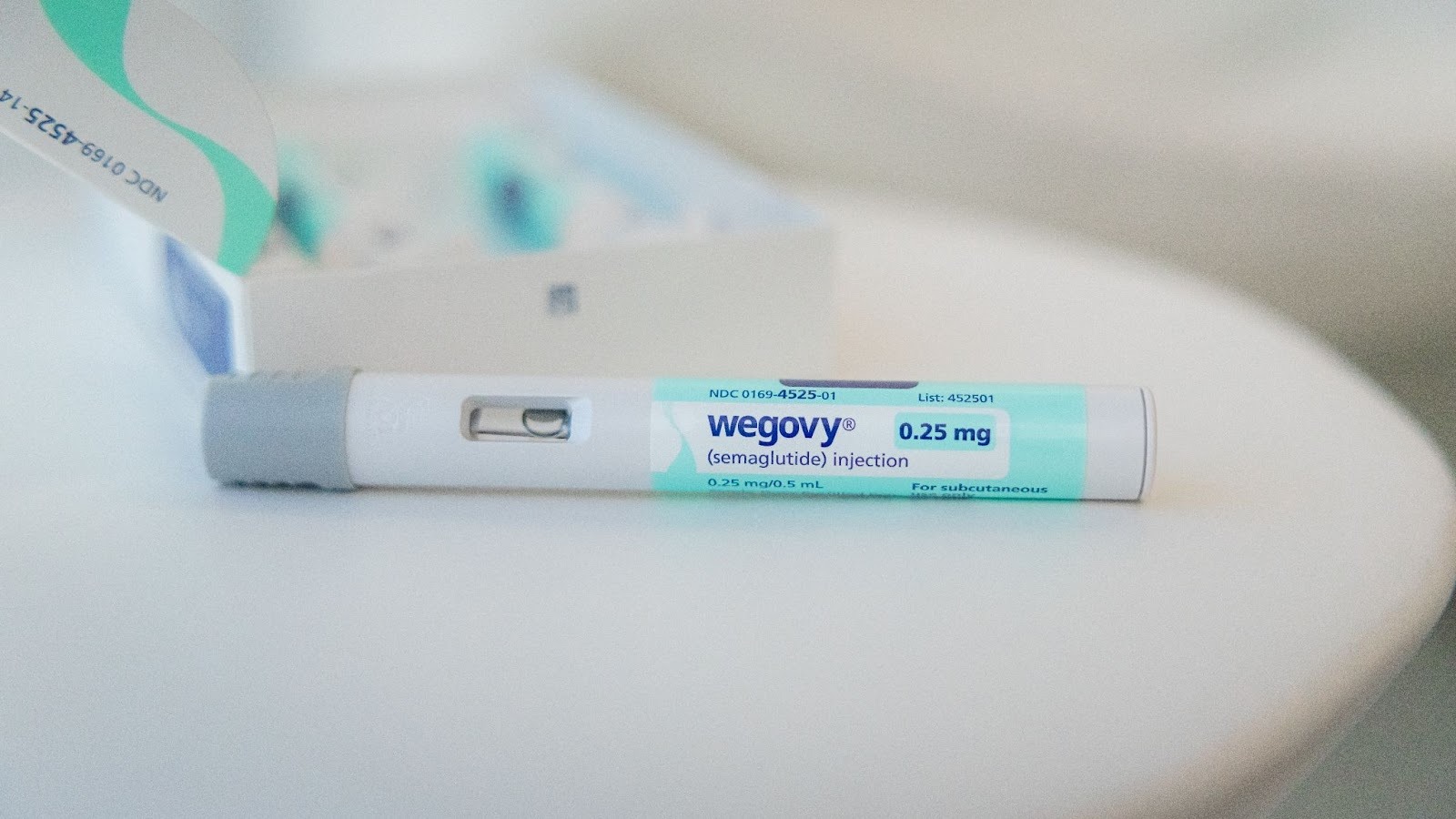
What Are GLP-1 Medications?
GLP-1 stands for glucagon-like peptide-1, a hormone your body naturally produces.
It helps regulate blood sugar, slows digestion, and signals to the brain that you are full. GLP-1 medications are designed to mimic this hormone and amplify those effects.
As a result, individuals taking these medications often experience reduced appetite, eat less, and see improvements in blood sugar control.
These medications were originally developed for type 2 diabetes. Their impact on weight, including average reductions of 10% to 15% in clinical trials, is what expanded their use and brought them into broader clinical and employer conversations, as reported in the New England Journal of Medicine study on semaglutide.
Why Is Demand Rising So Quickly?
The increase in demand is not happening in isolation. It is being driven by a combination of awareness and access.
More people are seeing visible changes in weight and metabolic health, which naturally leads to more conversations. Clinical trial data has demonstrated significant weight reduction associated with GLP-1 medications, including findings published in the New England Journal of Medicine.
At the same time, awareness has expanded beyond clinical settings. Employees are hearing about GLP-1s from peers, social channels, and everyday discussions.
Access has also become more widespread. There are now more pathways for individuals to seek out these medications, which accelerates utilization. For employers, this creates a new dynamic. Interest is growing rapidly, often before a clear strategy is in place to manage it.
How Do GLP-1 Medications Work?
GLP-1 medications influence three key areas. They reduce hunger signals in the brain, help individuals feel satisfied with less food, and slow the rate at which food leaves the stomach.
They also support blood sugar regulation by influencing insulin and glucose levels. Together, these effects create sustained changes rather than short-term appetite suppression.
What Happens After Someone Starts a GLP-1
It is easy to assume that the most important step is getting access to the medication. In reality, the more important phase begins after treatment starts.
An employee may begin a GLP-1 with clear expectations based on what they have seen or heard. Early changes can feel encouraging, particularly as appetite shifts and initial progress becomes visible.
Over time, however, the experience becomes more complex. Doses typically increase, and side effects may need to be managed. Guidance from the FDA emphasizes the importance of gradual dose escalation and ongoing monitoring during treatment.
Progress can become less predictable, and questions arise about what is normal and what to expect next. Some individuals adjust and remain consistent with treatment. Others pause, stop, or restart later. These differences are not unusual.
The Difference Between Starting and Staying on Treatment
There is a meaningful distinction between starting a GLP-1 and staying on it long enough to see sustained results.
Starting treatment is a single decision. Continuing treatment requires ongoing engagement and support.
As individuals move forward, they must navigate dose changes, manage side effects, and adjust expectations over time. Research published in the Journal of Managed Care & Specialty Pharmacy shows that long-term adherence is a key driver of outcomes across chronic therapies.
Without guidance, this process can become difficult to maintain.

Why This Matters for Employers
When employees start GLP-1 medications but do not remain on them, the impact is not neutral.
Costs are incurred early, but long-term benefits may not follow. Weight and metabolic improvements are often not sustained, and individuals may cycle on and off treatment.
At a population level, this creates a disconnect. Utilization increases, but outcomes remain inconsistent, and spending rises without clear long-term value.
Most large employers report concern about the cost and appropriate use of GLP-1 medications, particularly as utilization rises and outcomes vary, based on the Business Group on Health employer survey findings.
This is where the issue shifts from utilization to management.
What Happens Without a Structured Approach
As demand for GLP-1 medications increases, variation in outcomes becomes more visible.
Some employees achieve strong results. Others disengage early. The level of clinical oversight often depends on how treatment is accessed, leading to inconsistent experiences.
As a result, utilization rises without clear visibility into what is driving outcomes.
Without a structured approach to GLP-1 management, outcomes remain inconsistent and employer healthcare costs become harder to predict and control. This is where most employer strategies fall short.
Access Is Not the Same as Strategy
Much of the conversation around GLP-1 medications has focused on access. Can employees obtain these medications?
That question only addresses the first step.
A more complete employer strategy considers how GLP-1 treatment is managed over time. It includes decisions about who is appropriate for treatment, how progress is monitored, and how outcomes are defined and measured.
When these elements are not clearly addressed, programs tend to become reactive. When they are aligned, it becomes easier to connect GLP-1 utilization with outcomes and manage employer healthcare costs more effectively.
What This Comes Down To
GLP-1 medications are getting attention because they produce visible results.
But the medication itself is only one part of the equation.
What ultimately determines impact is how these medications are supported, managed, and integrated into a broader approach to population health and chronic condition management.
That distinction defines whether GLP-1s remain a reactive cost or become a managed strategy.
Disclaimer: This blog is maintained by eMed for informational purposes only. Content published here does not constitute medical, legal, financial, or benefits advice and should not be relied upon as such. Third-party statistics, studies, and research cited are sourced from publicly available data and provided for general informational context only; eMed makes no representation as to their accuracy, completeness, or applicability to any specific employer population, and results may vary. eMed's GLP-1 program pairs FDA-approved, on-label medications with clinical oversight; individual health outcomes depend on a variety of clinical and personal factors and cannot be guaranteed.
Note Regarding Medical Perspectives: Any content contributed by eMed's Chief Medical Officer is provided in her personal capacity as a licensed physician for general informational purposes only. Such content does not constitute medical advice from eMed, establish a physician-patient relationship, or represent eMed's official clinical guidance. Readers should not act on any health-related information without first consulting a qualified healthcare provider.Employers and individuals should consult qualified legal, benefits, and medical advisors before making plan design, coverage, or healthcare decisions. eMed assumes no liability for decisions made based on information contained in this blog.
.jpg)
.jpg)
.jpg)
.jpg)